H2 Deck By Bold Name
h2 xxxxxx
H1 xxxxxx
h2 xxxxx

Management
As engineers inspect more complex geometries, validate software-based functions after release and monitor suppliers across global supply chains, they now expect quality systems to support faster innovation. By Genevieve Diesing
Medical Device Manufacturers Redefine Quality Amid Digital, Regulatory and Supply Chain Pressures
Medical
H2 Deck Info By Paragraph Style Bold
Headline
Medical device manufacturers are changing how they inspect devices, manage suppliers and evaluate performance over a product’s lifecycle.
Today, medical devices incorporate more complex geometries, software-based functions and globally sourced components. Inspection methods, validation approaches and oversight models that once centered on final checks and periodic audits no longer address how many devices are designed, built and supported.
As manufacturers take greater responsibility for defining and validating how complex medical devices are measured, engineers increasingly need to evaluate internal features, tight tolerances and complex assemblies that traditional gages cannot fully assess. To do so, quality teams now use methods such as computed tomography and multisensor coordinate measuring machines to examine characteristics that previously required destructive testing or could not be measured at all. Existing FDA and industry standards describe quality system requirements but offer limited direction on how to validate these newer inspection approaches, prompting manufacturers to define inspection protocols internally and document their rationale for regulators.
Paul Brackman, X-ray product manager at ZEISS Industrial Quality Solutions, said manufacturers cannot rely only on established standards as device designs evolve. “Medical devices are becoming more complex, and companies can’t afford to wait years for new standards to be developed,” Brackman said. As a result, manufacturers increasingly write their own inspection procedures and quality criteria rather than relying solely on FDA or ASTM standards.
Carrie Pfeifer, applications engineer at ZEISS Industrial Quality Solutions, said manufacturers often work directly with measurement equipment suppliers to establish validation approaches that fit their products and risk profiles. FDA standards outline what a quality management system must achieve, she said, but do not always explain how to apply advanced measurement technologies in practice. That leaves manufacturers responsible for demonstrating that their inspection methods produce reliable, defensible results.
Regulatory pressure also shapes how manufacturers approach quality beyond inspection and measurement. Ed Goffin, vice president of product marketing at Pleora Technologies, said suppliers and device makers are preparing for new European Union cybersecurity requirements that affect how devices are designed, secured and supported over time.
“One area we’re actively tracking as a supplier is the potential impact of European Union cyber resiliency requirements on development practices, product lifecycle security, and supply chain oversight,” Goffin said. “These regulations underscore the importance of designing medical devices with cybersecurity in mind. While full compliance is still a few years away, we’re already working internally and with customers to ensure our products meet EU standards.”

CT technology supports innovation in the medical industry by enabling comprehensive analysis of complex parts through digitalization.
Manufacturers increasingly invest in their own oversight
Manufacturers are also changing how they manage suppliers as device designs and supply chains become more distributed. Components, software and services now come from multiple tiers of suppliers operating across different regulatory environments. While many manufacturers still participate in annual audits and rely somewhat on supplier certifications, they increasingly verify incoming components and processes themselves to confirm ongoing compliance and reliability.
“While suppliers conduct quality control and certify outgoing parts based on specified requirements, it’s no longer enough to say the parts were good when they left the building,” Brackman said.
Broader access to digital quality data has changed how manufacturers assess supplier risk, Pfeifer said. Quality teams can now analyze performance trends across sites and suppliers instead of reviewing issues in isolation. Statistical tools that once required specialized expertise are more widely available, allowing manufacturers to identify early warning signals and apply consistent decision rules across their supply base.
Many manufacturers are moving away from uniform oversight models, said Sai Ranjith Ramakrishnan Kumar, digital device quality engineering lead, Sanofi. Instead, they segment suppliers based on factors such as component criticality, regulatory exposure and performance history. “Traditional annual audits cannot adequately address today’s risks,” he said. Continuous, risk-based monitoring allows quality teams to focus resources where failures would have the greatest impact on production and patients.
Global disruptions have reinforced that approach. Pandemic-related shutdowns, trade restrictions and regional instability pushed manufacturers to adopt dual-sourcing and regional diversification strategies. Those changes reduce reliance on single suppliers but increase the need for ongoing visibility into quality performance, delivery reliability and compliance status.
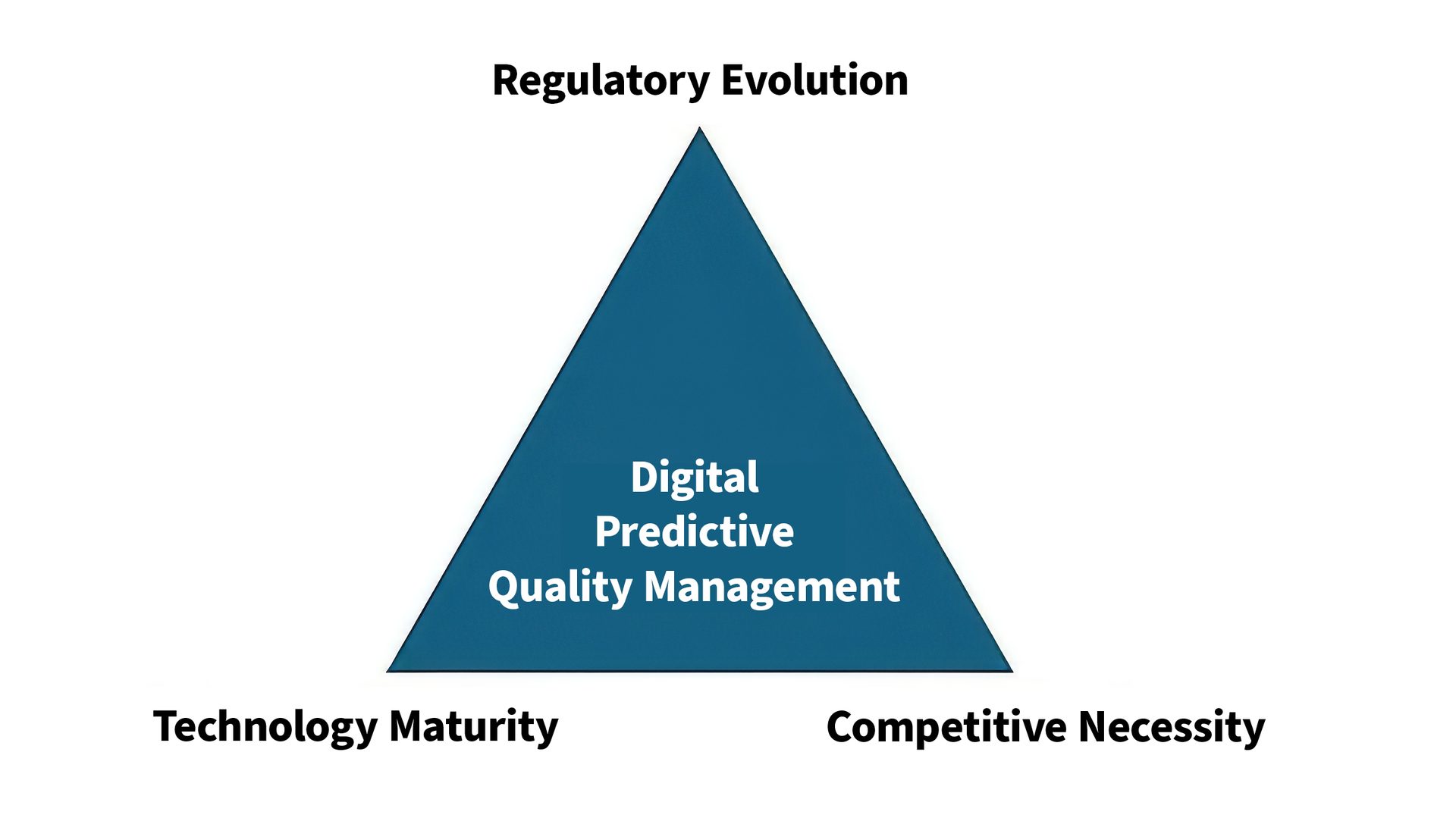
The shift toward digital and predictive quality management is driven by three converging forces: regulatory expectations, technological capability and competitive necessity.
Performance evaluation extends beyond manufacturing release
Some medical devices rely on software to perform key functions. Quality teams therefore continue reviewing device performance after release instead of treating approval as the final checkpoint.
Quality teams must actively monitor devices in use when software, AI-enabled features or connectivity influence how those devices perform, said Kumar. He said FDA guidance now expects teams to validate performance continuously and review real-world data rather than relying on one-time verification during premarket testing.
“Regulatory and market pressures are driving a fundamental redefinition of quality in medical devices—from compliance-focused to outcome-driven,” Kumar said. “The FDA’s evolving guidance on AI/ML-enabled devices and Software as a Medical Device requires continuous validation and real-world monitoring rather than one-time verification. Simultaneously, market pressures demand cybersecurity resilience, post-market transparency, and demonstrated patient outcomes beyond basic regulatory compliance.”
This change in evaluation affects how manufacturers define and use quality metrics. Traditional measures such as inspection pass rates and corrective action volumes remain relevant, but they do not capture how software-driven functions behave after deployment. Kumar said teams increasingly monitor indicators such as algorithm performance drift, software validation effectiveness and real-world device behavior to identify issues earlier.
Quality teams use digital systems to review inspection, manufacturing and post-release data together and spot early signs of risk or performance changes. When manufacturers apply that information during product development, teams can address problems earlier and reduce reactive investigations.
AI supports inspection, validation and documentation
Manufacturers also apply artificial intelligence selectively to support inspection, validation and documentation tasks, particularly where volume and repetition strain manual review.
As device geometries and assemblies become more customized, Brackman said manufacturers expect AI to play a larger role in inspection. “AI offers significant potential to improve inspection efficiency, particularly in identifying defects and analyzing intricate designs,” he said. At the same time, questions about validation and acceptability continue to shape how manufacturers deploy these tools in quality-related decisions.
Pfeifer said manufacturers approach AI cautiously because quality and regulatory expectations remain high. While AI may work well in processes with standardized inputs and outputs, she said its role in less predictable scenarios remains limited. “The medical device manufacturing industry places a special emphasis on quality, responsibility and regulatory requirements, and AI adoption must align with these standards,” Pfeifer said.
Kumar said manufacturers use AI to support quality work rather than replace human judgment. “AI is transforming quality processes by augmenting human capabilities with greater speed and consistency,” he said. In inspection, AI can review images or verify component placement and flag anomalies for human review. In validation, AI can analyze large data sets from testing to identify patterns across samples. Documentation tools can also assist with drafting procedures or reviewing supplier certificates, provided manufacturers validate those tools and monitor their performance.
Quality teams remain responsible for validating AI systems and determining when human expertise must override automated output, Kumar said.
Quality expectations expand across the lifecycle
As inspection practices, supplier oversight and performance evaluation change, manufacturers increasingly manage quality across a device’s lifecycle rather than relying on isolated checkpoints.
Brackman said manufacturers face growing challenges around unused or disconnected data. Companies that implement connected quality systems to unify and analyze information across devices, processes and facilities can make decisions faster and respond more effectively as conditions change. He said those systems also help manufacturers keep pace with the speed of modern manufacturing as inspection and analysis demands increase.
Pfeifer said the underlying definition of quality remains the same, but how manufacturers meet requirements continues to evolve. “While the fundamental definition of quality as the degree to which requirements are fulfilled is unlikely to change, the nature of those requirements and how medical device manufacturers rise to meet them will evolve significantly,” she said.
Kumar said connected and software-enabled devices expand quality considerations beyond physical attributes verified at manufacturing. “Quality is evolving from a static product attribute verified at manufacturing to a dynamic performance characteristic maintained throughout a device’s lifecycle,” he said. For AI-enabled devices, teams must monitor algorithm performance over time and across patient populations. Connected devices also introduce cybersecurity resilience, interoperability and data integrity as ongoing quality considerations.
Traditional manufacturing metrics such as first-pass yield remain useful, Kumar said, but they do not capture these dimensions. Teams increasingly evaluate real-world effectiveness, user experience and long-term reliability alongside traditional measures.
Quality functions take on a broader role
Taken together, these changes place greater responsibility on quality organizations. Engineers and quality teams increasingly shape inspection strategies, supplier relationships and post-release monitoring rather than focusing only on compliance documentation.
Manufacturers that integrate quality data into product development and decision-making can identify issues earlier and respond before problems escalate. That approach also supports more resilient supply chains and smoother regulatory interactions.
As devices incorporate more software, connectivity and global sourcing, quality systems continue to adapt. Manufacturers now align inspection, supplier oversight and performance evaluation with how devices are designed, built and used, extending quality management well beyond the factory floor.
Images Source: ZEISS Industrial Quality Solutions and Sai Ranjith Ramakrishnan Kumar
Genevieve Diesing is a contributing editor to Quality
READ MORE:

